The following is an excerpt from "Isolation isn’t new for those with intellectual disabilities. But covid-19 still poses a threat," an op-ed by Timothy Shriver for the Washington Post. The original article can be read here.
What our society looks like after this crisis depends on our collective understanding of the threats posed by inequity — and the work we do to address them. Let’s start by recognizing that people with intellectual disabilities are among those most vulnerable to the novel coronavirus. This is partly because about a quarter of adults with intellectual disabilities in the United States live in group homes. The risk of infection and death in these environments is staggeringly high. A recent study of group homes and similar facilities in New York City estimated that residents are around five times more likely than the general population to develop covid-19, and that those who get it are about five times more likely to die from it.
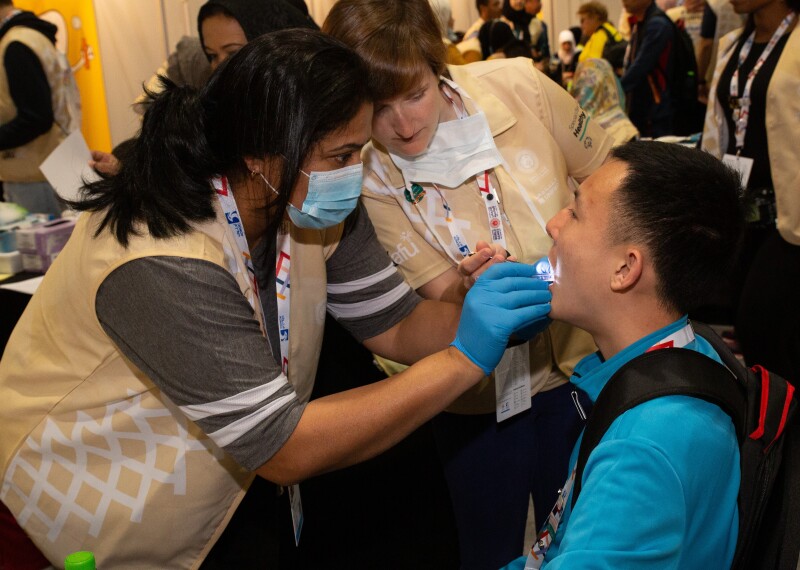
For a host of reasons related to being a medically underserved population, people with intellectual disabilities already suffer disproportionately from preventable disease, chronic pain and premature death. We have yet to resolve inequalities in our health-care system that are causing death, illness and emotional trauma to those who were already marginalized. Health-care providers and support staff must be trained to work with people who have intellectual disabilities — not just during the pandemic but all the time. This kind of training has long been lacking. More than 80 percent of medical students reported receiving no clinical training in the care of patients with disabilities in a 2009 study by the American Academy of Developmental Medicine and Dentistry. Health-care providers must know how to effectively communicate about covid-19 prevention, how to recognize symptoms and, more broadly, how to treat people with intellectual disabilities.